It happened again. A 14-year-old boy with a known peanut allergy ate a granola bar at school, showed signs and symptoms of anaphylaxis, and did not survive.
Allergic reactions to food are common at school. One in 12 children come to school with a food allergy. Of those, 18% have at least one reaction within the span of two years.
Anaphylaxis is an acute, life-threatening allergic reaction to a substance to which the body has become hypersensitive. It usually involves food, insect venom, medication or latex.
Mild allergic reactions do occur. A few hives or an eczema rash may appear – these are common mild symptoms. An itchy nose, mouth or eye symptoms and some stomach discomfort are also typical mild symptoms.
Treatment for a mild allergic reaction varies. Usually a medical professional prescribes an antihistamine and there is time to wait to see if things get better.
Anaphylaxis is different. It is typically diagnosed when severe allergy symptoms affect two or more body organs. Anaphylaxis can be difficult to identify in the school setting. For someone with a known allergy, when the following symptoms are seen, think anaphylaxis:
- Skin: hives that pop up and spread across the body; swelling on the lips or tongue; tightness or swelling that affects swallowing or breathing
- Lungs: uncontrollable cough, wheeze, shortness of breath
- Head, Eyes, Ears, Nose and Throat: runny nose, sneezing, swollen eyes, hoarse voice, phlegmy throat
- Stomach: vomiting, diarrhea, cramping
- Heart: Pale skin; blue-tinged lips or fingernails; a faint, weak pulse; feeling dizzy
- Other: confusion, agitation, feeling of doom
Ask the Allergist video: potentially life-threatening food allergy reactions
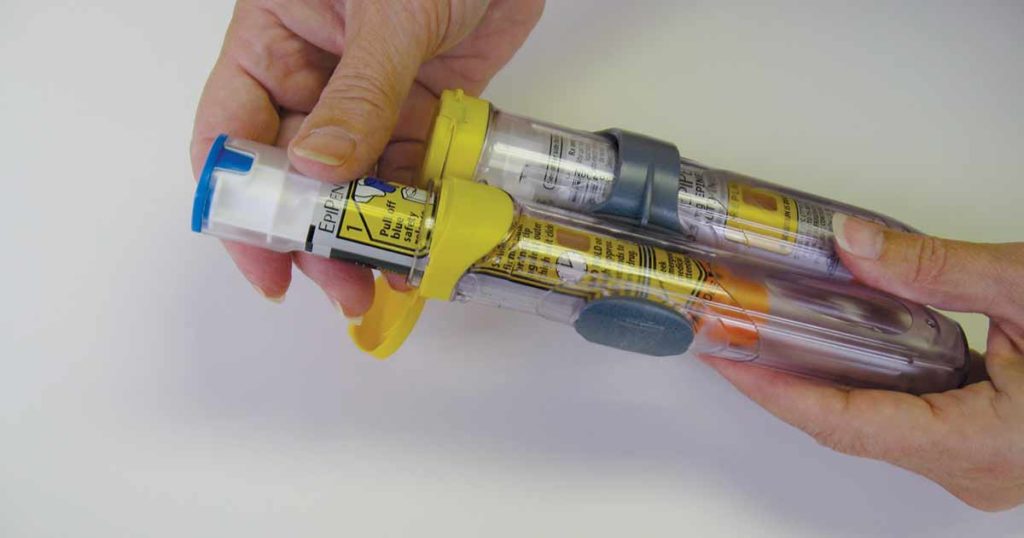
Treatment for anaphylaxis needs to be immediate. The first and only treatment is epinephrine. There is no other drug. Just one. Talk with your doctor about a prescription for an epinephrine auto-injector.
Epinephrine Infographic Transcript
What is Epinephrine?
Epinephrine, also called adrenaline, is a naturally occurring hormone in your body that is part of your body’s fight-or-flight response. Epinephrine will stop the symptoms of anaphylaxis – a life-threatening allergic reaction.
What does epinephrine do?
- Increases heart rate and blood pressure
- Relaxes muscles that are blocking the airways
- Increases blood flow through veins by narrowing blood vessels
- Reverses swelling
- Suppresses the body's response to allergic reactions
Epinephrine is safe to use for most people. It is the first line of defense to treat anaphylaxis.
What are the common side effects of epinephrine?
- Increased heart rate
- Talk with your doctor about using epinephrine if you have heart disease. Anaphylaxis is a life-threatening condition and epinephrine is the only treatment. Epinephrine is short-acting, so it will not cause long-term effects on the heart
- Looking pale
- Palpitations
- Shaking
- Nervousness
How should epinephrine be stored?
- Store at room temperature - avoid extremely hot or cold temperatures
- Extreme heat or cold can make the epinephrine less effective and/or cause the device to malfunction.
- Do not store in a car or in direct sunlight.
Epinephrine Helpful Tips:
- Learn how to correctly use the epinephrine auto-injector device prescribed to you. Each brand has different operating instructions.
- Each brand of epinephrine auto-injector contains different doses – learn which is right for those at risk for anaphylaxis.
- Check to see if the liquid in the device is clear. If it’s cloudy, replace the device.
- If you only have an expired epinephrine device during an emergency, it’s OK to use it as it may provide some help. Seek emergency medical help immediately afterwards.
- Keep your auto-injectors in a secure but easy-to-find place.
- You should always have 2 auto-injectors available in case you need more than one dose before medical emergency first aid arrives.
- If symptoms don’t improve in 5 or more minutes, administer a second dose if possible.
If you need to use epinephrine:
- Learn the signs and symptoms of anaphylaxis and how to use your device.
- Be prepared to treat anaphylaxis - develop an Anaphylaxis Action Plan.
- Don't delay: Epi-first, Epi-fast!
- If you are unsure if you need epinephrine - use it!
- Someone who has just received epinephrine should lay down with legs elevated. Do not rise to a sitting or standing position. If vomiting, lay on the side.
- Seek hospital care. Epinephrine can buy you time to get to a hospital for further treatment.
- A second reaction may occur – this is called a biphasic reaction. It may require a second dose of epinephrine.
A respected allergist once said, “If you say to yourself, ‘I wonder if I should give the…‘ and ‘epinephrine’ is the next word, don’t finish the sentence – give the epinephrine.” The risk is not in giving epinephrine, it is in DELAYING the use of epinephrine.
If someone dies from anaphylaxis, it is usually due to the delay in administering epinephrine.
We don’t know all of the circumstances in this latest tragic death from anaphylaxis. We do know that school nurses and school staff need to be ready to respond to an allergic emergency.
School nurses, teachers, coaches and other school staff should be trained to…
- identify anaphylaxis signs and symptoms
- use an epinephrine auto-injector in an emergency
Allergy & Asthma Network has food allergy management resources available to assist school nurses and staff.
Preschool and daycare workers also need to be aware of food allergies. New York, Illinois and Virginia adopted Elijah’s Law to require daycares to develop guidelines for identifying and preventing anaphylaxis. This includes training and strategies to reduce exposure to food allergens.
Pennsylvania and California are considering versions of Elijah’s Law. If you live in those states, you can get involved by telling your legislator to support the legislation.
Patient Story: Why Minutes Count with Anaphylaxis
The following was written by Sandra Fusco-Walker, Allergy & Asthma Network’s Director of Outreach from 1996-2003 and Director of Patient Advocacy from 2003-2013.
As a patient advocate for 20+ years, I’ve met so many families who have lost loved ones to anaphylaxis. Those who died had one thing in common. They didn’t use epinephrine. Either they weren’t aware they had a severe allergy and never had a prescription, they forgot to carry it, or they thought they did not need it anymore.
National guidelines emphasize epinephrine is the first line of treatment for anaphylaxis. Using it makes the difference between life and death … and minutes count.
My mantra as an advocate was always, “When in doubt, give the shot!” The medication won’t harm you if you really don’t need it – but anaphylaxis will, and it just might save your life.
In the back of my mind, I wondered about the qualifier that medical professionals added when I asked about safety … “Epinephrine won’t kill them, but if they have a weak heart, maybe an older person – epinephrine might be a problem.”
On July 19, 2014, I knelt beside my 63-year-old husband, Scott, the only one in our family with no history of allergies or anaphylaxis. He was writhing on the ground drenched in sweat. He was retching and barely conscious 10 minutes after some yellow jackets stung him.
I held an epinephrine auto-injector in my hand and hesitated. Even though all the symptoms were there, right in front of me, I started questioning myself. Should I wait for the ambulance? Should I give him the shot? Is his heart strong?
I remembered the ending to those conversations about safety – “If they’re already dying from anaphylaxis, a heart attack doesn’t really matter, does it?” – and I plunged the device into my husband’s thigh. I counted off 13, my lucky number.
As I pulled the device away, I watched the red rash on Scott’s arms solidify to blotches. Ten minutes later, EMTs arrived with more epinephrine and gave him a second shot. By the time Scott entered the emergency room, he was lobster red from his head to his feet. Except for his fingers and toes – they looked black, apparently from the lack of oxygen in his blood.
The emergency department team worked their magic. Later the doctor told us it was the quick use of epinephrine that saved Scott’s life.
We are grateful to everyone who taught us so much at Allergy & Asthma Network. I’m especially grateful to those families who, despite their grief, bravely shared their experience in the hope that others wouldn’t lose their loved ones, too.
Your message was loud and clear. And it saved a life.
Reviewed by:
Purvi Parikh, MD, FACAAI is an adult and pediatric allergist and immunologist at Allergy and Asthma Associates of Murray Hill in New York City. She is on faculty as Clinical Assistant Professor in both departments of Medicine and Pediatrics at New York University School of Medicine.






 810304 Eaton Place, Suite 100
810304 Eaton Place, Suite 100