VCD – Vocal Cord Dysfunction
- Home
- |
- Health A to Z –...
- |
- VCD – Vocal Cord Dysfunction

What is VCD?
Vocal cord dysfunction (VCD) can look and feel a lot like asthma. It’s a condition in which your vocal cords close instead of opening as you inhale.
You can’t see your vocal cords in a mirror, but you can feel them. Put your hand on the front of your throat and swallow. That hard ball that moves up and down when you swallow is your voice box, or larynx. Vocal cords are folds of tissue that stretch across your voice box.
As you breathe in, your vocal cords open to let air go through into your lungs, then narrow as you breathe out. If you have VCD, your vocal cords suddenly close when they’re not supposed to, cutting off your air supply. Often this occurs during exercise or when you’re emotionally upset or crying – just when you need air the most.
What are VCD triggers?
VCD can be set off by factors often associated with asthma, including:
- Exercise
- Stress
- Cigarette smoke
- Perfume and other strong scents
- Upper respiratory infections
- Air pollution
- Cold air
Who has VCD?
Overall prevalence of vocal cord dysfunction is not known, but small studies indicate it is common in teenagers, particularly females who play sports that involve intense running. Some believe this is due to the effect of puberty on the developing larynx.
What are the symptoms of VCD?
Symptoms include:
- Wheezing or stridor (a high-pitched sound)
- Chronic cough or throat clearing
- Shortness of breath
- Upper chest or throat tightness
- Intermittent hoarseness
How Is VCD diagnosed?
The most accurate way to identify VCD is to use a laryngoscope – a flexible tube with a tiny camera inserted down the back of the throat to view the vocal cords. However, it must be done while symptoms are actually occurring. Doctors have patients exercise on equipment to induce symptoms, then use a spirometer to measure patient lung function. When VCD is occurring, the spirometer reading will show very different results from those seen with asthma.
VCD may be linked to chronic irritation of the throat making vocal cords sensitive. The irritation could come from postnasal drip caused by chronic nasal and/or sinus congestion or from gastroesophageal reflux, where stomach acids leak up into the esophagus.
How is VCD treated?
Beyond treating an underlying throat irritation such as gastroesophageal reflux disease (GERD), there is no specific medication available to treat VCD. However, many patients are referred to a speech pathologist.
A speech pathologist can help VCD patients learn to create muscle memory in the larynx to normalize breathing, especially during physical activity. For example, athletes with VCD must learn to breathe with their jaw relaxed and mouth open, using small, rapid inhalations and then exhaling through pursed lips.
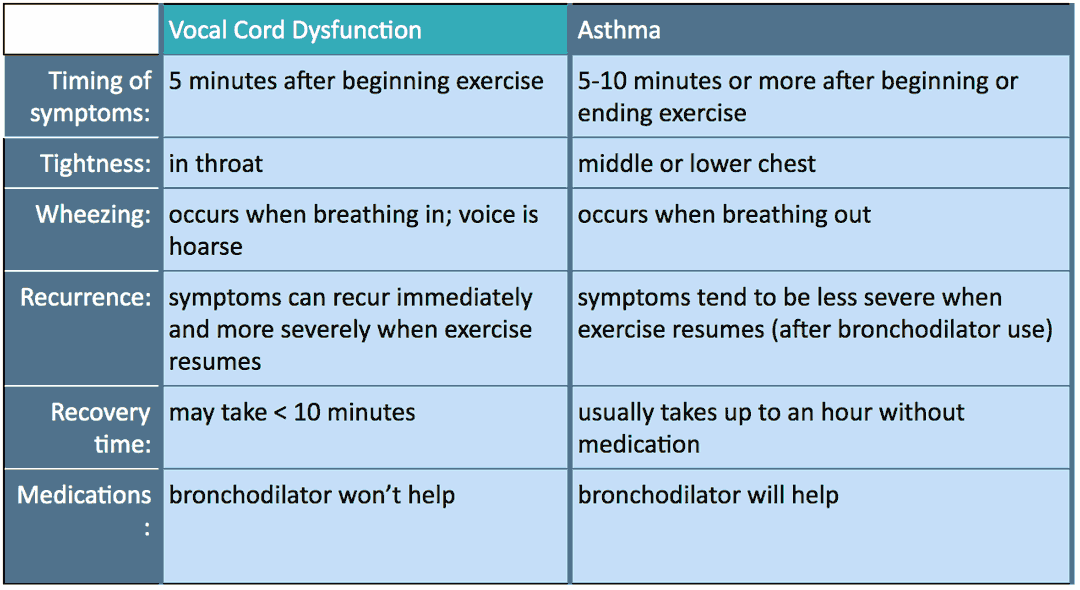
What is the difference between VCD & asthma?